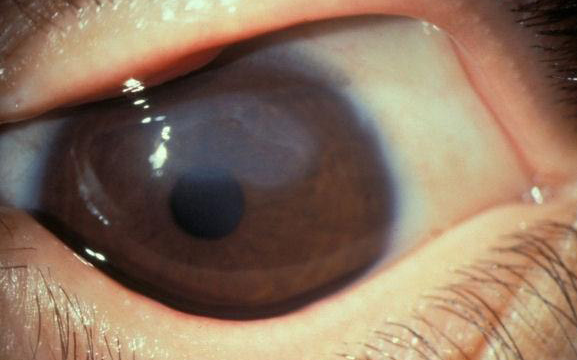
Conjunctivitis
What is conjunctivitis?
Conjunctivitis is an inflammation of the conjunctiva (the outermost layer of the eye). It is one of the most common eye diseases.
What are the symptoms of acute conjunctivitis?
Usually acute conjunctivitis begins suddenly. Patient complains about:
- Feeling of foreign body in the eye;
- Grittiness;
- Redness of the eye;
- Discharge from the eye;
- Watering;
- Swelling of the eyelid.
Acute conjunctivitis lasts from 3-4 days up to two weeks. Usually process occurs in both eyes - initially disease begins in one eye but after 3 to 4 days it affects also the other eye.
What are the forms of conjunctivitis?
Forms of acute conjunctivitis can be divided after aetiology into:
- Bacteria conjunctivitis;
- Viral conjunctivitis;
- Allergic conjunctivitis.
How conjunctivitis is diagnosed and treated?
Conjunctivitis can be diagnosed only clinically. Treatment is initiated without special bacteriological or virology examinations. But if acute conjunctivitis can't be cured with classic treatment methods, additional examinations are required to specify initiator of the disease. Delayed and incorrect treatment of acute conjunctivitis can turn into chronic form and torture both patient and doctor for years. In separate cases retina and deeper covers of the eyeball are involved in the process, thus creating worsening of vision.
In case of bacterial and viral conjunctivitis a routine is very important to prevent infection of other people around. Most important rules of personal hygiene:
- Do not touch your eyes with unwashed hands;
- Always wash your hands after you have touched your eyes;
- Provide regular ventilation in the premises;
- Provide regular cleaning-up of the premises, especially concentrating on the cleaning of door-handles and backrests of the chair;
- Don't put bandage on the eye because bacteria will multiply more actively in the warm, moist and closed place;
- Regularly wipe of discharges that comes from the eye with the cotton pad soaked into boiled water or strong infusion of tea.
Always contact doctor when acute conjunctivitis symptoms appear to establish diagnosis and determine treatment - usually disinfecting drops or ointments. Patient should take into consideration that frequently disregarding the started therapy, illness can progress on its own course and during the second and third day of the illness symptoms could be more explicit than during the first. If prescribed medications do not provide improvement after three - four days then therapy should be changed and additional examinations should be carried out.
How to avoid conjunctivitis?
To avoid conjunctivitis you should:
- Always wash hands before and after touching your eyes;
- Do not rub eyes;
- Do not use pillows, towels, cosmetic tools used by other people;
- Avoid contact with the patients of acute conjunctivitis;
- Before the first usage of unknown cosmetics (for example, mascara, shampoo, soaps etc.) always make sure that it does not cause allergic reactions.
Allergic conjunctivitis
What is allergic conjunctivitis?
Allergic conjunctivitis is one of the most common types of conjunctivitis that has been treated both in children and adults. It is often called “pink eye”. Allergic conjunctivitis is an inflammation of eye conjunctiva or transparent membrane/ocular mucosa. Eye conjunctiva covers the front part of the eyeball and the inside of eyelids, keeping them moistened.
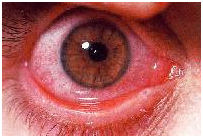
„Pink eye” in the case of allergic conjunctivitis
In the case of inflammation of ocular mucosa, the common complaints are itchy eyes, eyelid swelling, watering, photophobia, watery or mucus-based discharge and feeling of foreign bodies in the eye. The most common symptom of the eye allergy is itching that is experienced by over 75% of patients with allergic conjunctivitis. Allergic conjunctivitis is not contagious.
What are the causes of eye allergy?
Allergens that cause conjunctivitis can be located both indoors and outdoors. Household dust, dust mites, pet dander are the most common indoors allergens. Indoor allergens may cause the symptoms throughout the year resulting in chronic allergic conjunctivitis. The most common outdoors allergens are grass, trees and weed pollen. People who are sensitive to these allergens suffer from seasonal allergic conjunctivitis that is the most common type of eye allergy. Allergic reactions in the human body may be caused also by mould spores, medications (including eye drops), cosmetics, food products, insect bites. Cigarette smoke, odours and exhaust fumes may act as irritants that cause allergic symptoms, or may worsen allergic reaction.
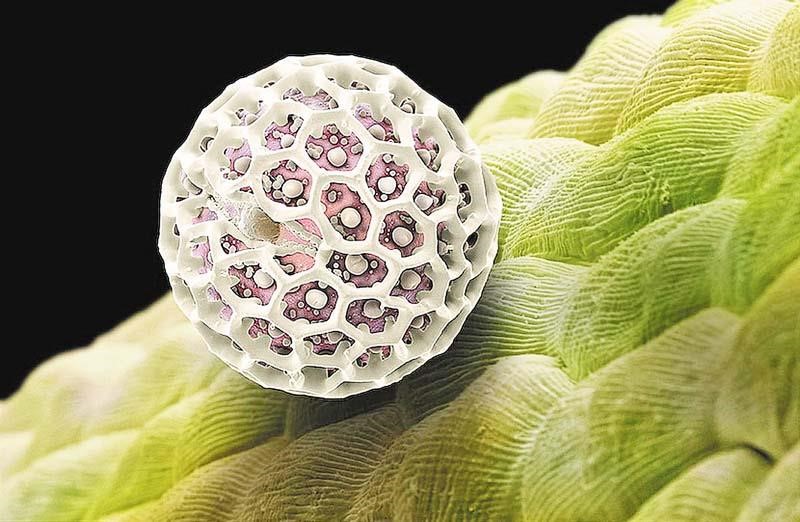
Plant pollen – electron microscope image

Dust mite – electron microscope image
Allergy as an immune system error
Atopy – an allergic reaction of an organism caused by irritating factors, characterised by genetic reaction and susceptibility. Responses of an immune system occur on the surface of the eye forming antigens that enter the bloodstream and can cause inflammation of conjunctiva. As a result, activation of immune system occurs and a cytotoxic reaction, formation of immune complexes, as well as cell activation reaction occurs. During the allergic reaction, histamine is released from mast cells and the inflammatory reaction occurs immediately. For delayed allergic reactions, the immune system responds within about 8-24 hours.
Any allergic reaction is based on an inadequate response of the immune system: to “protect” the organism, it destroys its own tissues and cells. The first contact with an allergen causes the formation of large number of IgE class antibodies (rarely -IgG4). These antibodies bind to mast cells and basophils. When the allergen re-enters the body, it is recognized by the antibodies on the cell surface, the cells are activated and a large number of molecules are produced that cause allergic symptoms and tissue damage around the contact point of allergens – histamine, heparin, serotonin, platelet activating factor, prostaglandins, leukotrienes, etc.
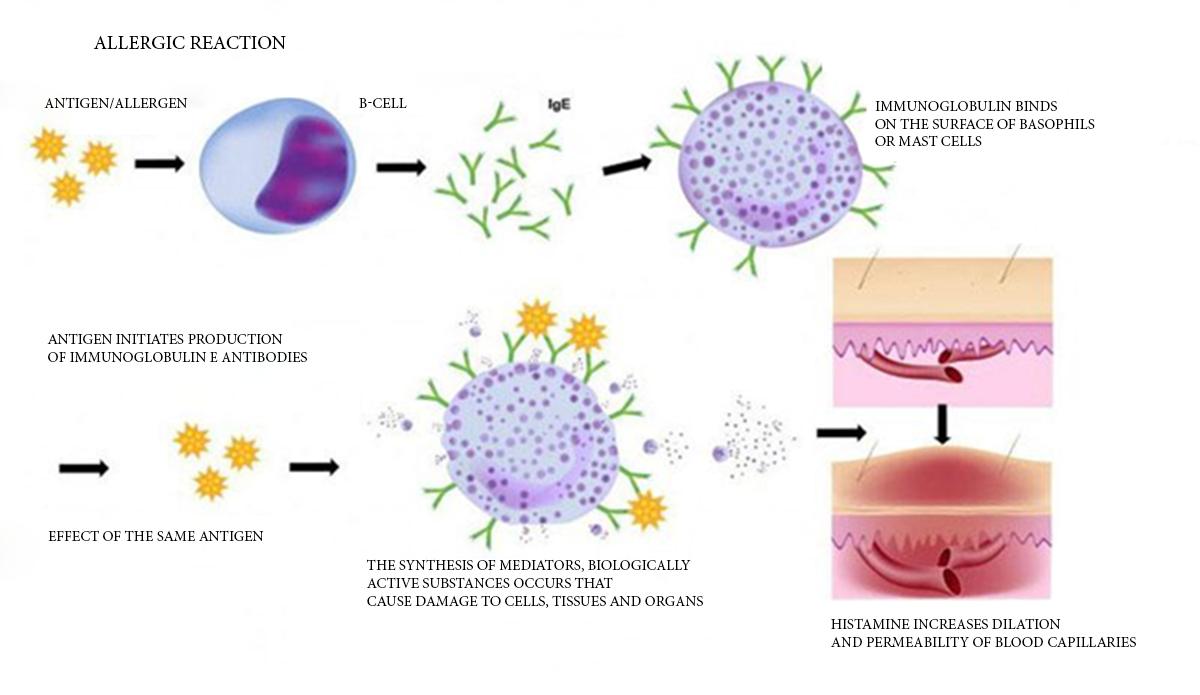
Schematic description of allergic reaction
What are the types of allergic conjunctivitis?
Seasonal allergic conjunctivitis and perennial allergic conjunctivitis are often grouped in the light acute allergic conjunctivitis or hay fever conjunctivitis group. Seasonal allergic conjunctivitis occurs every year at the same time. The most cases are associated with “hay fever”. The term “hay fever” refers to a set of allergic manifestations resulting from meadow herb and weed pollen during the summer period in June, July and August.
Other sub-types of allergic conjunctivitis –vernal keratoconjunctivitis, atopic keratoconjunctivitis and giant papillary conjunctivitis – form the group of perennial conjunctivitis.
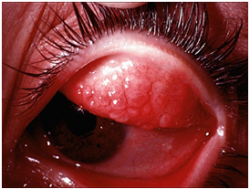
Papillary allergic reaction of the conjunctiva of upper eyelid
Shield ulcer of the cornea in the case of keratoconjunctivitis
Atopic keratoconjunctivitis is caused by allergens that may come into contact with cornea, for example, cosmetics, medications, etc. In cases of severe eye allergy, such as vernal keratoconjunctivitis or atopic keratoconjunctivitis when the cornea is affected, failure of timely diagnosis and appropriate treatment may endanger vision.
How allergic conjunctivitis is treated?
In practice, the use of antihistamines (soft cells stabilizers) as a maintenance therapy, continued by pulse therapy with topical steroids during exacerbations. Corticosteroids are effective in treating allergic conjunctivitis. However, the profile of side effects (cataract, glaucoma, herpes infection, corneal ulceration) makes it unpopular choice over the long term. Corticosteroids must only be used under the supervision of eye specialist.